by developmentdruttamspecial | Jul 3, 2022 | Blog, Dermatologist In Kolkata, Skin Care
INTRODUCTION
Hidradenitis suppurativa is a chronic inflammatory skin disease.
It occurs due to infection of apocrine sweat glands of the hair follicles, causing painful boils (pus filled bumps), nodules, cyst and sinus tract formation over the skin.
Sites affected : Mostly in the area of skin folds i.e.
- Axilla (armpits)
- Groin
- Thighs
- Buttocks &
- Under the breasts
WHO CAN DEVELOP (EPIDEMIOLOGY)
Hidradenitis suppurativa is seen to occur more in females than in males.
It usually occurs during Puberty, and rarely in childrens and adults.
CAUSES & MECHANISM
The exact cause of this disease is not known.
However, there are multiple risk factors that are associated with this condition :-
- Obesity
- Smoking
- Excessive sweating
- Wearing tight fitting dresses
It starts with the infection and inflammation of the apocrine sweat glands and its ducts, along with ‘Follicular Keratosis’, which means blockage of the hair follicle.
The sweat gets accumulated under this blockage, leads to painful tender pus filled bumps / boils over the skin. This may burst, causing more inflammation, nodules, cyst & sinus tract formation.
Upon healing, it leaves huge scars over the skin.
CLINICAL FEATURES / SYMPTOMS
- Recurrent boils in the areas of skin folds (mentioned above) – These areseverely painful and associated with oozing of pus as well as
- Huge scar formations – due to repeated appearances of boils over the same area of the skin folds and recurrent healing. Scarring leads of painful restriction of movement and depression.
- It can prevent people from going out frequently, wearing their favorite clothes etc. Hence, it severely affects the quality of lifestyle.
DIAGNOSIS
Hidradenitis suppurativa can be diagnosed byclinical examination and History taking of the patient.
The patient usually presents with a history of recurrent boils.
A characteristic finding in Hidradenitis suppurativa is ‘Double comedones’ i.e. a papule containing two black-heads, commonly in the axilla.
Other findings includes cysts, nodules, sinus tracts etc. which helps in confirming the diagnosis.
PREVENTION AND TREATMENT
- General measures
- Avoid risk factors which aggravate the disease, such as :-
- Obesity – lifestyle modification
- Avoid smoking
- On Excessive sweating, bathe thorougly and keep the body surface dry, especially in the areas of skin folds.
- Avoid tight fitting clothes, which may cause increased sweating. It is preferable to wear loose cotton clothes.
- Proper cleaning of the pus, oozing out from the infected areas, followed by proper dressing.
- For excessive pain, painkillers can be used.
- Chronic cases of Hidradenitis suppurativa can cause the patient to be depressed, which also needs to be addressed.
- Medications
- Topical antibiotic creams
- Erythromycin cream
- Azithromycin cream
- Fusidic acid cream
- Benzoyl peroxide
- Mupirocin cream etc.
- Oral antibiotics – These are used in long term therapy
- Rifampicin
- Clindamycin (combined with Rifampicin is found to be very effective against Hidradenitis suppurativa)
- Doxycycline
- Minocyclin
- Tetracycline
- Erythromycin
- Isotretinoin capsules are effective. It is also used in treatment of pimples.
- In case of large cysts, incision of the cyst and drainage is performed.
- Intra lesions Steroid injection
- Some other drugs have been found to be effective in this condition, which are currently in trial phase:-
- Zinc
- Cyclosporin
- Anti androgen
- Oral contraceptive pills
The above medicines/drugs/procedures have been found to be effective in the treatment of Hidradenitis suppurativa. However, not all drugs are suitable for every patient.
The appropriate drug of choice, its dosage and duration is best prescribed by a professional clinician.
It is advised to consult your doctor before starting any medicine.
- Monoclonal Antibodies / ‘Biologicals’ – These are the most recent advancement in the treatment of Hidradenitis suppurativa:-
- Infliximab
- Etanercept
- Adalimumab – used widely &USFDA approved; administered via subcutaneous injection
Monoclonal antibodies are one of the best methods of treatment, but is very expensive.
After the control of infection and inflammation by the above methods, hair removal and scar removal can be achieved by Laser therapy, such as CO2 laser. This leads to long term relief of the patient.
- Surgical Management- It is done in highly resistant and advanced stages of this condition. In such cases, surgery proves to be essential and curative.
In it, the sweat glands within the affected area are surgically removed. It leads to a permanent cure of this condition, without any chances of recurrence.
by developmentdruttamspecial | Jul 3, 2022 | Blog, Dermatologist In Kolkata, Skin Care
INTRODUCTION
Granuloma Annulare (GA) is a relatively uncommon skin condition, characterized by red/skin colored circular asymptomatic Rash with elevated borders and central depression, closely resembling ring worm.
WHO CAN DEVELOP (EPIDEMIOLOGY)
As mentioned earlier, it is a relatively uncommon skin condition/disease.
It is seen more commonly in children and in females.
Incidence after the age of 30 is rare.
It can be associated with Diabetes and thyroid problems.
CLINICAL FEATURES & SYMPTOMS
Cinical features of Granuloma Annulare (GA) includes :-
- Characteristic asymptomatic ring-rashes that are slightly elevated in the periphery and depressed in the middle.
- It can closely resemble ‘daad’ or ringworm infection.
GA rashes are mostly asymptomatic. Pain and itching is rarely seen in this condition. However, cosmetic problems and appearance of the skin is the major cause of treatment.
TYPES
- Localized GA – it appears in isolated areas of the body, mostly seen in the dorsum of Hand and foot.
- Generalized GA – It is characterized by multiple small rashes all over the body, which may combine to turn larger rashes. It appears more on the sun exposed part of the body.
DIAGNOSIS
- Diagnosis of GA can be done by simple clinical examination by any professional dermatologist.
- In a variant called papular Granuloma Annulare, the rashes appear different from the classical form. In such cases, Skin biopsy is done to confirm the diagnosis.
- GA is usually asymptomatic. So rarely, if a patient complains of pain and itching, KOH test is done to rule out fungal infection (ringworm)
In KOH test, the skin is gently scraped on the surface and a sample of the skin is collected and sent to the laboratory, to detect the presence of fungi.
TREATMENT
GA is normally self-limitingand resolves within 1-2 years.
However, various methods for prompt treatment are also available :-
- Steroid creams – High potency steroid creams like Clobetasol, Halobetasol, Mometasone.
- Intra lesions Steroid injection for rapid resolution.
- Oral medications – Dapsone, Isotretinoin, Hydroxy chloroquine, Niacinamide etc.
- In resistant cases (rashes do not go away easily, even on treatment), biological medications, such as Infliximab, Etanercept, Adalimumab can be used. However, these are very costly.
Granuloma Annulare is a chronic disease, and recurrence is common on old sites, even after resolution/treatment of previous rashes. However, the recurrent cases are easily curable and is not cause for much concern.

by developmentdruttamspecial | Jun 17, 2022 | Blog
INTRODUCTION
Acne Rosacea is a condition in which the skin becomes red, develops rashes and flushing i.e. the skin feels hot.
Most common area affected – Face
Other areas in the Scalp, Chest, Hands etc. can also be affected.
The symptoms of skin redness and itching usually intensify, when exposed to the sun.
SYMPTOMS
On the basis of symptoms, Acne Rosacea can be classified into 4 types:-
- TYPE I {Telangiectactic rosacea}: Most common type. It is associated with telangiectasis i.e. appearance of large dilated veins on the skin.
- TYPE II {Papulo–pustular rosacea}: It is associated with pus filled tiny white/red bumps over the skin. It can be commonly mistaken for acne.
- TYPE III {Rhinophyma rosacea}: It affects the Nose of the individual. It is a chronic long standing condition, in which the skin of nose appears rough and swollen like a potato, and its structure gets distorted; a condition called ‘Bulbous nose’. It’s the most severe form of rosacea.
- TYPE IV {Ocular rosacea}: The conjunctiva of the eye is affected. It’s associated with Red eyes, Gritty feeling in the eyes, pain and itching of the eyes. The patient may have difficulty seeing.
WHO CAN DEVELOP?
Rosacea normally appears after the age of 30, but rarely children are affected.
CAUSES
The exact mechanism behind this condition is not known yet.
However, there are multiple risk factors which are seen to be associated with this condition:-
- Genetic: It is seen in those persons, whose family members have been previously affected by it.
- UV Radiation: People who are exposed to the sunlight for long durations have been seen to be affected.
- Side effects of cosmetics OR use of strong steroid creams (clobetasol, halobetasol etc.)
- Skin infections such as Demodex follicularum (parasite), Staphylococcus epidermidis (bacteria)
- Alcohol
- Spicy foods
DIAGNOSIS
Acne rosacea can be diagnosed by clinical examination of the symptoms. And in some cases, Skin biopsy may be required.
One should look out for:-
- Red bumps
- Pustules (pus filled tiny bumps)
- Redness of skin
- Flushing (burning of skin)
Other diseases with similar looking symptoms are:-
- Acne
- Perioral dermatitis
- Gram negative folliculitis
Therefore, for proper diagnosis & treatment one must consult a dermatologist.
TREATMENT
- General measures
- Avoid heavy makeup, cosmetics.
- Avoid using strong steroid cream over the face.
- Use plenty of physical sunscreen, containing zinc oxide or titanium dioxide.
- Avoid hot and spicy food, alcohol.
- Medicines used? Creams like:-
- Azeleic acid cream
- Pimecrolimus cream
- Tacrolimus cream
- Metronidazole cream
- Sulphur cream
- Oral medicines:-
- Doxycycline
- Minocyclin
- Isotretinoin
- Ivermectine – Used in parasite induced rosacea
- Brimonidine gel; Xylometaxoline & Oxymetazoline cream can be used to treat skin redness.
- Laser treatment is useful in treating Telangiectactic rosacea & Rhinophyma (CO2 laser resurfacing)
- Surgery can be done in cases of Rhinophyma
Rosacea is a chronic disease. Its duration of treatment can be long. And recurrence has been seen in some cases, but it gets better by treatment. It’s important to have patience and carefully follow the doctor’s advice.
by developmentdruttamspecial | Jun 14, 2022 | Blog
INTRODUCTION
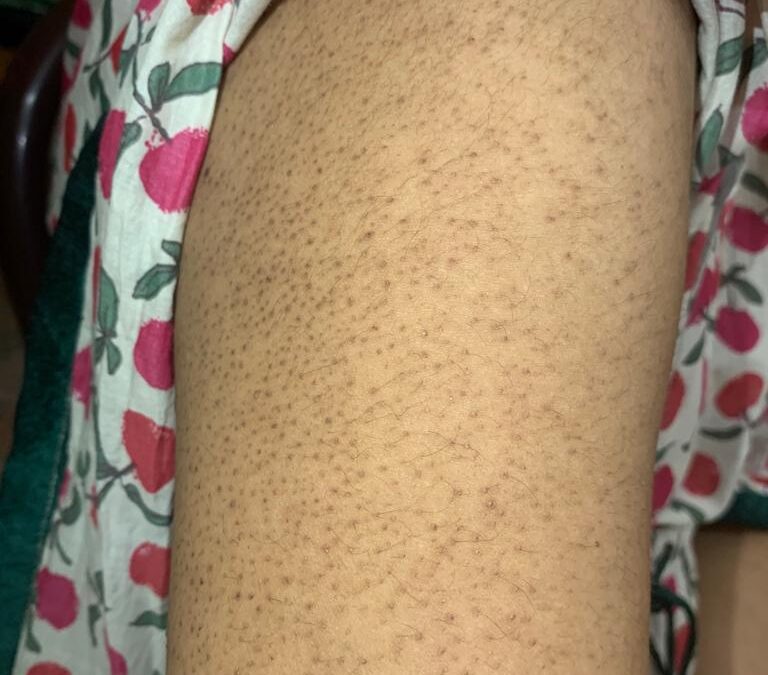
It is a condition where certain areas of the skin become dry and rough, with small bumps appearing in that area, resembling pimples.
Most common sites affected – Upper arms, thighs
Other sites affected – Forearms, legs, cheeks, or anywhere in the body having hair follicles
It is a non-contagious condition.
WHO CAN DEVELOP (EPIDEMIOLOGY)
Keratosis pilaris is most commonly seen in children and teenagers. And it appears to resolve on it’s own as one’s age progresses to mid 20s and 30.
SYMPTOMS
In Keratosis pilaris, no pain or itching is associated with the affected area.
However, the patient may face cosmetic problems :-
- Most notably skin pigmentation (change in skin color)
- The affected area may turn black, brown or red (in fair skinned people) depending on the skin color of the patient.
- Affected area has tiny bumps of the same color, resembling pimples.
CAUSE
In Keratosis Pilaris, keratin – a hair protein, accumulates over immature hair follicles and dead skin cells, which appears as tiny bumps over the skin.
The exact cause of accumulation of keratin is not known.
RISK FACTORS
- Genetic – It is commonly seen in people whose family members were affected with the same condition.
- Environmental – It appears more during dry seasons like winter, when the skin is prone to dry up.
- Age – children and teenagers are mostly affected
- Obesity
- It can be associated with other skin conditions such as Atopic dermatitis, Icthyosis etc. and other dry skin
DIAGNOSIS
Keratosis pilaris is a condition which can be diagnosed by any dermatologist by simple clinical examination.
It usually does not require any additional tests or investigations.
TREATMENT
There’s no permanent cure for this condition yet.
However many options for symptomatic cure are available, which restores the appearance of the skin :-
- Home remedies
- Use warm water for bathing.
- Short time baths – Because bathing for longer duration can cause skin dryness.
- Use moisturizer after bath.
- Physical exfoliator, like scrub can be effective in removing the keratin plugs.
- Avoid tight fitting dress.
- Use humidifier at home – to keep your skin cool and moist.
- Creams
- Keratinolytic agents (which breaks down keratin) such as
- Urea
- Lactic acid
- Salicylic acid
- Glycolic acid
- Retinoic acid cream (Trentinoin) etc., containing creams may be used for treatment.
*Caution / Contraindications (Note to patients)
- Avoid rubbing these creams in excess, which may cause burning, itching & redness over the skin.
- Retinoid creams are strong keratinolytics, but they should be avoided in pregnant or lactating mothers and those who are planning for pregnancy, because retinol is a teratogenic. Hence it can affect the baby.
Consult a Dermatologist for personalized details of these below therapies
3. Chemical peeling
4. Microdermabrasion
5. Laser treatment
by developmentdruttamspecial | Jun 14, 2022 | Blog
INTRODUCTION
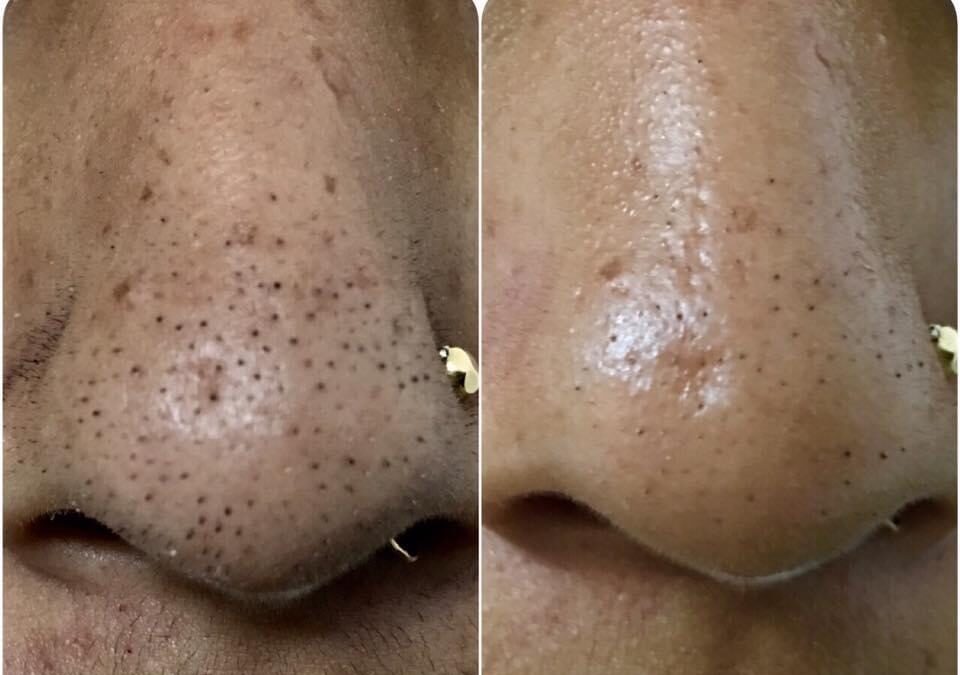
It’s a hair follicle disorder, characterised by spiny black papules containing multiple fine hairs, greatly resembling blackheads/pimples.
Each blackhead like point, when observed under a magnifying glass or dermatoscope, contains 5-25 fine hairs.
This condition is most commonly presented in the Nose.
Other sites of appearance may include – Scalp, Hand, Chest etc.
It can be easily confused with Blackheads/pimples, and the patient may apply multiple creams for it’s resolution. However, Trichostasis spinulosa cannot be treated with any medicated cream.
WHO CAN DEVELOP (EPIDEMIOLOGY)
Any age group, and both males and females can be affected.
SYMPTOMS
Most notable symptom in Trichostasis spinulosa are the cosmetic concerns that the patient usually presents with.
Otherwise, it is asymptomatic.
CAUSE
Trichostasis spinulosa occurs due to growth of multiple telogen club hairs from a single hair follicle.
The exact mechanism behind this is not known.
RISK FACTORS
- Skin damage
- Other skin diseases
- Aging etc.
DIAGNOSIS
- It can be diagnosed by a dermatologist by simple clinical examination.
- Dermatoscopy (magnification) is useful in diagnosis.
- No other tests are required.
TREATMENT
- The fine hairs/hair follicles can be removed by tweezers or comedon extractors.
- Plucking, Waxing& Nose strips can also help in removing the hair follicles.
However, by the above methods of treatment, there are high chances of recurrence.
Therefore, other methods such as :-
- Advanced hair removal laser treatment, combined with
- Retinoid cream (Trentinoin) can be used for long lasting results.































